Keywords:
Abdomen, Computer applications, CT-Quantitative, CT, Computer Applications-General, Technical aspects, Metabolic disorders, Endocrine disorders, Mesentery
Authors:
M. M. BARIS, A. PEKER, A. S. Yener, N. S. GEZER, M. Secil; Izmir/TR
DOI:
10.1594/ecr2018/C-2653
Methods and materials
Study Participants
Patients who have been admitted to Endocrinology Department of Dokuz Eylul University for the investigation of incidentally discovered adrenal tumours between 2008 and 2017 were included in our study.
Patients with adrenocortical carcinomas,
metastasis or active malignancy were excluded.
A concomitant endocrinological investigation identified nonfunctioning adrenal adenomas,
subclinical Cushing's syndrome or Cushing's syndrome in recruited individuals.
CT investigations of these patients were selected.
130 patients were found according to these criterias.
One patient was excluded who has CT of positron emission tomography (PET) investigation with different CT parameters.
Routine CT investigations of 129 patients were evaluated retrospectively.
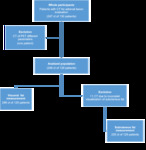
246 abdominal CT of 129 patients were evaluated with QCT.
246 measurements for visceral fat evaluation were performed.
11 CT was excluded from the subcutaneous fat measurement group due to lack of visualization in the peripheral zone of abdominal subcutaneous fat in morbidly obese patients.
235 measurements for subcutaneous fat evaluation were performed.
Totally 481 measurements were performed (Fig.
1).
Fat measurement method
An axial view was used with the subject lying in the supine position.
The fat compartment areas were measured on Philips Extended Brilliance Workspace (software version V3.5.0.22.54) using QCT (quantitative computed tomography) software.
L1/2 disc space was identified for fat measurements because visceral adipose tissue (VAT) at the T12–L1 and L1–L2 landmarks had much stronger associations with metabolic syndrome than measurements at other sites (7).
A region of interest (ROI) with a size of 100-200 mm2 was drawn on the para-renal compartment of visceral fat to determine the reference HU values for fat area measurements.
An attenuation range of -60 to -165 HU was observed.
Using this ROI as a density reference for fat,
the software automatically provided fat tissue area values.
Total adipose tissue area (TAT) was measured by drawing a contour around the skin.
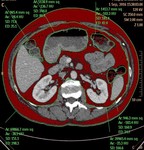
Another contour was drawn around the visceral fat by identifying the innermost part of the abdominal wall muscles and anterior aspect of the vertebral column to determine Visceral Adipose Tissue (VAT).
Subcutaneous fat was defined as the area of adipose tissue between the skin and the outermost aspect of the abdominal muscle wall.
The Subcutaneous Adipose Tissue (SAT) area was calculated by subtracting VAT area from TAT area.
Each intestinal intraluminal false positive highlighted areas in VAT measurement slice were selected and additional ROI areas were drawn around the intestine lumen to exclude intestinal intraluminal falsely highlighted areas from total VAT measurement (Fig.
2).
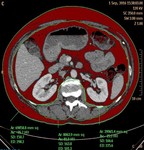
With the same method,
an additional ROI was drawn around the fat in paraspinal muscles in the same slice to exclude from SAT (Fig.
3).
Statistical Analyses
For evaluation effect of falsely highlighted intestinal intraluminal areas and additional fat compartments in paraspinal muscles, two methods (method 1: including falsely highlighted intestinal intraluminal fat to VAT measurement and including fat in paraspinal muscles to SAT measurement,
method 2: excluding falsely highlighted intestinal intraluminal fat from VAT and excluding fat in paraspinal muscles from SAT) were compared statistically.
Difference between measurements with two different methods (including and excluding accessory highlighted areas) was tested on medcalc software.
Statistical analyses for evaluation of the correlation between two methods were performed using spss version 15.0 (SPSS Inc,
Illinois,
USA).
Intra-and interindividual variability between two investigators performing fat area measurements was tested on medcalc software (Ostend,
Belgium).
To assess interindividual variability,
74 consecutive CT images were evaluated by both investigators (Inv1 vs Inv2).
To assess intra-individual variability,
each investigator (inv) measured fat areas in 18 consecutive CT images 6 months apart (Inv1a vs Inv1b and Inv2a vs Inv2b).
Passing and Bablock regression analysis indicated strong agreement between measurements (Inv1 vs Inv2,
Inv1a vs Inv1b and Inv2a vs Inv2b; the 95% CI for the intercept A contains the value 0 and the 95% CI for slope B contains the value one in all regression models).
Regression coefficient was >0.9 and P value was <.001 in all regression models.